
Chronic pain is like an unwanted guest that overstays its welcome. It’s the kind of pain that hangs around, often for months or even longer, regardless of whether an injury has healed. Unlike acute pain – the body’s natural alert system that warns us of injury – chronic pain doesn’t just shut off when the threat is gone. It persists, becoming a complex condition in its own right.
In my opinion, to grasp the enormity of chronic pain, it’s essential to recognize its prevalence. It’s a silent epidemic, according to the CDC, 20.9% of US adults, or 51.6 million people, experienced chronic pain in 2021, affecting a substantial portion of the population, often leading to significant lifestyle changes, mental health issues, and increased healthcare costs. Common triggers for chronic pain include arthritis, fibromyalgia, and nerve damage. Sometimes, chronic pain is a mystery without an obvious physical source, making it even more challenging to treat.
Understanding chronic pain isn’t just about the ‘ouch’; it’s also about exploring the biopsychosocial model. This approach considers how the interplay between biological factors, psychological state, and social environment contributes to the pain experience. It underscores that pain isn’t merely a symptom; it’s an intricate personal experience influenced by various aspects of our lives.
Now, explaining this pain to others and healthcare professionals is crucial, which leads us to the next section. You’ll discover the art of communicating about pain that often seems indescribable. Whether it’s pinning down the right words or picking a number on a pain scale, the better you can convey what you’re experiencing, the closer you are to finding some relief.
The Language of Pain: Communicating Your Experience Effectively
An integral part of dealing with chronic pain is learning how to express what you’re going through. It’s not just about giving it a number on a scale; it’s about conveying the impact it has on your life to those around you and to healthcare professionals who can help. Precise communication can lead to better understanding and treatment.
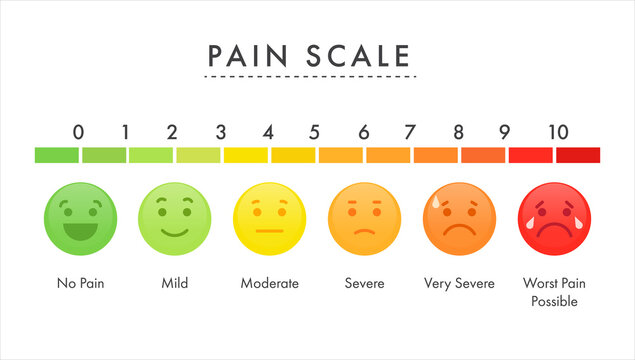
Now what are these pain scales I’m talking about? Healthcare providers often use them as tools to measure pain intensity. One common example is the numerical rating scale where you rate your pain from 0, no pain, to 10, the worst pain imaginable. But pain is complex, and sometimes numbers fall short.
You might find it more illuminating to describe your pain. Words like ‘throbbing’, ‘shooting’, ‘burning’, or ‘aching’ paint a clearer picture. If metaphors speak to you, compare your pain to something familiar. Maybe it feels like an unrelenting vice grip or a persistent, heavy cloak that you carry around.
Keeping a pain diary can be a game-changer. You’d jot down the severity of your pain, its location, and triggers – which gives your doctor a reliable history instead of a one-off description. It’s a thorough way to capture the fluctuations and patterns over time.
So why is this important? Effective communication can open doors to better pain management. Now, let’s discuss how to make others understand your experience with chronic pain – a key step in maintaining healthy social relationships and getting the support you need.
I’m going to tackle one of the trickier parts of living with chronic pain: social interactions. This isn’t just about opening up; it’s also about setting boundaries to manage expectations and maintain healthy relationships.
Here are some strategies and tips to help you communicate your experience effectively:
1. Use Simple Analogies and Comparisons: 
Analogies can make the invisible visible. Compare your pain to something familiar to the person you’re talking to.
For example:
- “Imagine having a constant toothache, but it’s in your back and legs instead.”
- “It’s like carrying a heavy backpack all day, every day, no matter what I’m doing.”
2. Be Honest and Direct:
- Clearly explain your limitations without sugar-coating the situation. Honesty helps others understand the severity of your condition.
- Example: “I would love to join you for the hike, but my chronic pain makes it difficult for me to walk long distances. I need to listen to my body and rest.”
3. Set Boundaries and Manage Expectations:
- Establish clear boundaries about what you can and cannot do. This helps prevent misunderstandings and ensures that others know how to support you.
- Example: “I might have to leave the gathering early if my pain flares up. I hope you understand that it’s not because I don’t want to be there.”
 4. Use Descriptive Language:
4. Use Descriptive Language:
- Use specific and descriptive words to articulate your pain. Words like “throbbing,” “burning,” “stabbing,” or “aching” can help others visualize your experience.
- Example: “My pain feels like a sharp, stabbing sensation that doesn’t go away. It’s especially bad in the mornings and evenings.”
5. Share Your Pain Scale:
- Utilize pain scales to quantify your pain. While numbers alone may not capture the full experience, they provide a starting point for discussion.
- Example: “On a scale of 0 to 10, my pain is usually around a 6, but it can spike to an 8 or 9 on bad days.”
6. Explain the Impact on Daily Life:
- Describe how chronic pain affects your daily activities, work, and social interactions. This helps others see the broader impact of your condition.
- Example: “Chronic pain makes it hard for me to concentrate at work and sometimes I have to take breaks to manage the discomfort.”
7. Emphasize the Unpredictability:
- Chronic pain can be unpredictable, with good days and bad days. Explain this variability to help others understand why you might cancel plans unexpectedly.
- Example: “Some days I feel relatively okay, but on other days the pain is overwhelming, and I need to rest. It’s unpredictable and can change from hour to hour.”
8. Educate About the Condition: 
- Provide basic information about your specific condition. This can help dispel myths and increase understanding.
- Example: “I have fibromyalgia, which means my body processes pain differently. Even minor activities can cause severe pain and fatigue.”
9. Encourage Questions:
- Invite others to ask questions. This shows that you’re open to discussing your condition and helps build empathy.
- Example: “Feel free to ask me anything about my condition. I know it can be hard to understand, and I’m happy to explain.”
10. Use Visual Aids:
- Sometimes, visual aids like charts or diagrams can help illustrate your pain points and the areas affected.
- Example: Show a diagram of the body highlighting the areas where you experience pain, or use an app to track and share your pain levels.
11. Seek Support from Allies:
- Identify supportive friends or family members who can help explain your condition to others, especially in social or work settings.
- Example: “My friend Sarah knows a lot about my condition. If you have any questions, she can also help explain what I go through.”
12. Practice Self-Compassion: 
- Remember that it’s okay to prioritize your well-being. Don’t feel guilty for setting boundaries or needing support.
- Example: “I need to take care of myself to manage my pain. Thank you for understanding that I might need to sit out certain activities.”
Example Dialogue:
- You: “I really appreciate you inviting me to the picnic. However, I have chronic pain, which means I have to be careful about how much I exert myself.”
- Friend: “Oh, I didn’t realize. What does that mean for you day-to-day?”
- You: “It’s like carrying a heavy weight all the time. Some days it’s manageable, but other days, even simple tasks can be overwhelming. I might need to rest more or leave early if my pain gets worse.”
The impact of chronic pain isn’t always obvious, which leads to misunderstanding. Sharing what you can and cannot do makes it easier for others to appreciate the daily challenges you face.
Talking openly about your experiences also sheds light on the psychological battle with chronic pain. The stigma is real, but the right conversation can challenge misconceptions and foster a deeper sense of empathy from others.
Now, I understand that these conversations are never easy. But by being clear and consistent in your approach, you can navigate social situations with more confidence and less anxiety.
Seeking Support and Advocacy: Building a Network for Management
Chronic pain can feel like a solitary struggle, but it doesn’t have to be. Building a support network is key in managing your pain effectively. Don’t hesitate to reach out to support groups; they can offer empathy from others who truly understand your experience. You can find these groups online or in your community—your healthcare provider may have recommendations. 
Self-advocacy is crucial in dealing with chronic pain. When you’re dealing with healthcare professionals, be clear and assertive about your needs. Remember, you’re the expert on your own pain. Don’t be afraid to ask questions about treatments or pain management strategies.
Knowledge is power when it comes to tackling chronic pain. Familiarize yourself with resources such as pain clinics, pain management programs, and rehabilitation services. Be proactive about the latest research and potential therapies.
Lastly, remember that managing chronic pain is often more successful with an interdisciplinary approach. Combining medical treatment with therapies like physical therapy, counseling, or acupuncture could provide comprehensive relief. It’s about finding what combination works best for you—and that might mean adjusting your strategy over time.
Support Groups for Family Members
Supporting a loved one with chronic pain can be challenging and isolating. Fortunately, there are support groups available specifically for family members:
- The American Chronic Pain Association (ACPA):
- Offers resources and support groups for families of individuals living with chronic pain.
- ACPA Support Groups
- Pain Connection:
- Provides virtual support groups for chronic pain sufferers and their families.
- Pain Connection Support Groups
- Family Caregiver Alliance (FCA):
- Offers online support groups and resources for family caregivers, including those caring for individuals with chronic pain.
- Family Caregiver Alliance
- Chronic Pain Anonymous (CPA):
- Offers support groups modeled after the 12-step program, with some groups including family members.
- Chronic Pain Anonymous
- Online Communities:
- Facebook groups like “Support for Families of Chronic Pain Sufferers” and subreddits like r/caregivers provide community and support.
- Search for these groups on Facebook or Reddit and request to join.
Conclusion
By effectively communicating your chronic pain experience and utilizing available resources, you can foster understanding, build supportive relationships, and manage your pain more effectively. Remember, you are not alone – there are communities and resources available to support both you and your loved ones.
JOIN OUR COMMUNITY ON FACEBOOK


This is a thoughtful and comprehensive guide to explaining chronic pain to loved ones! The tips on using analogies and descriptive language are constructive, especially when communicating something as complex as chronic pain. I also appreciate the section on setting boundaries and managing expectations, essential in maintaining relationships. One thing I’m curious about is how to approach the conversation when a loved one is struggling to understand or even believe in the severity of the pain. Do you have any suggestions for handling situations where there’s scepticism or misunderstanding?
Thank you so much for your kind words, Vlad! I’m glad you found the guide helpful, especially the sections on using analogies and managing expectations. When it comes to dealing with skepticism or misunderstanding, it can definitely be one of the more challenging aspects of communicating about chronic pain.
A lot of these illnesses are ‘invisible’ which leads to that very area of skepticism. There seems to be a stigma attached to these illnesses. Patient not only have to plead their case with loved ones, but oftentimes, with healthcare professionals as well. It becomes extremely disheartening.
One approach I recommend is starting with empathy—acknowledging that it can be difficult for someone who hasn’t experienced chronic pain to fully understand it. Sometimes, sharing personal stories or using relatable examples (like comparing pain to something they might have experienced, like a bad toothache or sprained ankle) can help bridge that gap.
It’s also important to express how their belief or support impacts your emotional well-being. You could say something like, “I know it might be hard to grasp what I’m going through, but your understanding means a lot to me.” If needed, inviting them to join you at a doctor’s appointment can also offer some external validation and a clearer picture. My doctor agreed to speak with my children who were all younger when this started and he was able to bring it ‘down’ to their level. I, also, invited only those that I was closest to come to support meetings with me. Then, when I actually started running a support group (with help from a therapist), I encouraged everyone in the group to bring their loved ones.
Thanks again for your thoughtful comments, and feel free to ask any questions at any time! I am always happy to help.
Warmest Regards,
Courtney