Chronic pain isn’t just a symptom; it’s a complex and persistent condition that can significantly impact one’s quality of life. Imagine your body’s alarm system never shutting off, constantly signaling distress, regardless of an immediate cause. That’s the daily reality for individuals living with chronic pain. It’s crucial to approach this topic with sensitivity and understanding. Pain is subjective, and what might be a minor inconvenience for one person can be debilitating for another. This isn’t just about physical discomfort. It’s also about the emotional and social toll that long-term pain can impose on someone’s life.
As we delve into the multifaceted world of chronic pain, we explore not only the medical side but also the very human stories behind the diagnoses. Real-life examples are key to appreciating the nuance of each condition and the perseverance of those who live with pain every day.
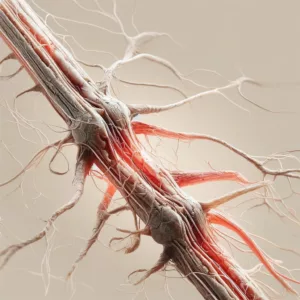
Understanding the various types of chronic pain is the first step in demystifying this condition. Our exploration will begin with neuropathic pain – a type that arises not from physical injury but from nerve damage. It’s a condition that can confound both sufferers and healthcare providers alike.
You’re going to learn about the journeys of people who cope with neuropathy, the struggles they endure, and the strategies they employ to manage their pain. Their experiences provide a valuable framework for what’s to come in the next section, as we continue to dissect the categories of chronic pain and the real-life implications for those affected.
Imagine a pain that’s hard to pinpoint, often described as a burning, shooting, or electric shock sensation. That’s neuropathic pain for you. It arises when nerves are damaged, dysfunctional, or injured, sending incorrect signals to other pain centers.
You might know someone who has it, or maybe you’ve read about it, but real-life examples bring this type of pain closer to home. Let’s talk about Jane, who developed neuropathic pain after her car accident. Despite the bruises healing, Jane still feels an unexplained burning sensation in her leg.
Or consider Alex, who fights a silent battle with diabetic neuropathy. To Alex, it’s not just about managing diabetes but also dealing with the tingling and numbness in the feet that make simple activities, like walking, an ordeal.
I’ve seen countless stories where people trudge on, grappling with a pain that is often invisible to others. And that’s just it – neuropathic pain often goes unrecognized, and that can be incredibly isolating.
What resonates with people like Jane and Alex is the need for understanding and the right management strategies. From medications tailored for nerve pain to therapies like TENS or nerve blocks, there’s a spectrum of ways to deal with neuropathic pain. And remember, support groups aren’t just about emotional solace; they’re also about swapping practical advice with those who truly understand your situation.
The Dual Aspects of Nociceptive Pain: Somatic and Visceral Explained
Now, let’s unpack nociceptive pain, which can be split into two main types: somatic and visceral. Understanding these two can really change how you address and treat your pain. 
Somatic pain is the ‘ouch’ you feel when you stub a toe or cut your finger. It’s sharp, usually well-localized, making it easier to tell exactly where the pain is coming from. This is the most common type of nociceptive pain.
Visceral pain, on the other hand, is trickier. It comes from internal organs and can feel more like a deep squeeze, ache, or pressure. It’s often harder to pinpoint and can refer pain to other parts of the body, which sometimes makes it a diagnostic puzzle.
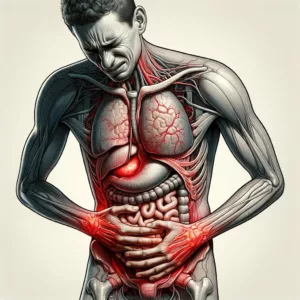 Think about the last time you had a cramp or a stomachache – that discomfort was most likely visceral pain. It’s less straightforward than somatic pain, often requiring more complex treatment approaches.
Think about the last time you had a cramp or a stomachache – that discomfort was most likely visceral pain. It’s less straightforward than somatic pain, often requiring more complex treatment approaches.
Both somatic and visceral pains are important signals. They’re telling you that something is not right. Whether it’s inflammation from an injury or an ongoing issue like arthritis or IBS, paying attention to these pains is crucial.
Treatment varies greatly. For somatic pain, it might include over-the-counter medications, physical therapy, or rest. Visceral pain often calls for a more investigative approach involving medications, diet changes, and sometimes even surgery.
Remember Jim from Section 2 with neuropathic pain? Imagine now Sarah, who has been learning to manage her somatic pain following a knee surgery, and Mike, who’s coping with visceral pain due to chronic pancreatitis. Their stories of perseverance and tailored treatments shed light on the nuance needed in battling nociceptive pain.
The Enigma of Functional Pain: Recognizing Invisible Suffering
I’m going to clarify something that often mystifies both patients and doctors alike: functional pain. This isn’t just about physical symptoms; it’s also about the challenges that come with a condition that’s notoriously  difficult to pin down. Functional pain stands apart because it doesn’t have a clear cause, like an injury or inflammation. It’s a bit like a ghost in the machine of our bodies — present and affecting us profoundly, yet elusive to standard tests.
difficult to pin down. Functional pain stands apart because it doesn’t have a clear cause, like an injury or inflammation. It’s a bit like a ghost in the machine of our bodies — present and affecting us profoundly, yet elusive to standard tests.
So what does living with functional pain look like? Imagine waking up every day to pain that seems to come from nowhere — no injury, no illness, just pain. That’s going to include experiences like that of mine, it started in my 20’s when I had first started as a RN and was a new wife and mother. I had unexplained fatigue, pain and burning of my muscles plus other symptoms for years, affecting my job and social life. My multitude of enigmatic symptoms left doctors scratching their heads, stating that I was a “walking, medical anomaly”, yet my suffering was very real.
If you want to handle functional pain effectively, it’s crucial to explore a blend of approaches — something I’m here to help you with. Treatments range from medications to physiotherapy and, notably, psychological support. Why? Because the mind-body connection plays a pivotal role in functional pain. Initiatives that foster this connection, such as mindfulness and cognitive behavioral therapy, can make a world of difference.
Understanding Inflammatory Pain: Causes and Symptoms
Inflammatory pain occurs when the body’s immune system responds to injury or infection by releasing  chemicals that cause inflammation and swelling. This type of pain is commonly associated with conditions such as arthritis, tendonitis, and inflammatory bowel disease. Symptoms often include redness, heat, and swelling in the affected areas, along with a constant or throbbing pain that can significantly impact daily activities.
chemicals that cause inflammation and swelling. This type of pain is commonly associated with conditions such as arthritis, tendonitis, and inflammatory bowel disease. Symptoms often include redness, heat, and swelling in the affected areas, along with a constant or throbbing pain that can significantly impact daily activities.
Consider Maria, who suffers from rheumatoid arthritis. Despite her efforts to stay active, she often experiences painful flare-ups in her joints, particularly in her hands and knees. The inflammation makes it challenging for her to perform everyday tasks, underscoring the importance of effective management strategies for those living with inflammatory pain.
Understanding Psychogenic Pain: The Mind-Body Connection
Psychogenic pain is a type of chronic pain that is primarily influenced by psychological factors such as stress, anxiety, and depression. Unlike pain caused by physical injury or inflammation, psychogenic pain often lacks a clear medical origin, making it challenging to diagnose and treat. This type of pain highlights the powerful connection between the mind and body, where emotional distress manifests as physical discomfort. 
Consider Emily, who has been struggling with severe headaches and back pain for years. Despite numerous medical tests, doctors could not find a physical cause for her pain. It wasn’t until Emily started therapy to address her anxiety and depression that she began to notice a reduction in her pain levels. Her experience underscores the importance of addressing mental health in the management of chronic pain.
In some ways, it intersects with functional pain but also diverts into its unique path. It underscores the complexity of chronic pain and how mental health can significantly influence physical symptoms. Remember, recognizing the legitimacy of these pain experiences is a vital step in providing relief and understanding to those who endure them daily.
Embracing a Multifaceted Approach to Managing Chronic Pain
In my opinion, taming the beast of chronic pain isn’t a one-size-fits-all endeavor. As you’ve learned about the various types of chronic pain, from neuropathic to psychogenic, you now know that the battle is as much about understanding as it is about treatment.
You’re going to find out that managing pain is about combining various strategies. This can include medications, lifestyle adjustments, and mind-body techniques. Remember, your first attempt doesn’t need to be your last—you can always adjust your approach down the road.
Now, if you’re grappling with any of these five main types of chronic pain, know that validation is crucial. This isn’t just about acknowledging the existence of pain, it’s also about recognizing the emotional and psychological toll it takes. 
I’m here to help you understand that reaching out for support, be it professional help, community support, or educational resources, is a sign of strength, not weakness. And guess what? There are many out there ready to stand with you.
As we conclude, I really hope that this deep dive into the world of chronic pain enlightens you and offers some comfort. If you want to learn more or need assistance, don’t hesitate to reach out to healthcare providers, support groups, or even friends and family. And always choose something that resonates with you, because dealing with chronic pain is not just a physical journey, it’s a personal one too.
JOIN OUR COMMUNITY ON FACEBOOK